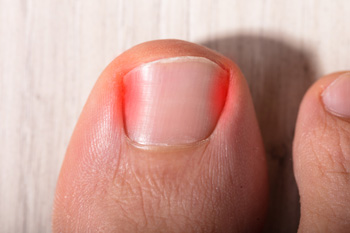
Ingrown toenails occur when the edge of a toenail grows into the surrounding skin, causing pain, redness, and swelling. The affected toe may become tender to the touch and appear inflamed. If left untreated, the area can become infected, and pus or drainage may develop. Most commonly, ingrown toenails affect the big toe, but they can occur on any toe. This condition is often caused by improper nail trimming, wearing ight footwear, or trauma to the toe. People with curved nails, or conditions like diabetes or poor circulation, are more prone to developing ingrown toenails. The pain can range from mild discomfort to severe, making walking or wearing shoes difficult. A podiatrist can help by carefully removing the ingrown portion of the nail, providing antibiotics if an infection is present, and offering advice on proper nail care and footwear. If you have a painful ingrown toenail, it is suggested that you schedule an appointment with a podiatrist.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. Richard DiMario of Maine. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Arthritis in the toes can cause significant discomfort and impact mobility. Swelling is a common symptom, often making shoes feel tighter and causing tenderness with pressure. Soreness may be persistent or worsen with activity, leading to difficulty walking or standing for long periods. Restricted movement can develop as the joints become stiff, making it challenging to bend or flex the toes. Additionally, redness and warmth surrounding the affected joints may indicate inflammation, often accompanied by pain. In more advanced cases, deformities such as bunions or claw toes can occur, altering the foot’s natural shape. The most common types of arthritis affecting the toes include osteoarthritis, rheumatoid arthritis, and gout. If you have toe pain, it is suggested that you confer with a podiatrist who can offer a proper diagnosis and treatment.
Toe pain can disrupt your daily activities. If you have any concerns, contact Dr. Richard DiMario of Maine. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
When to See a Podiatrist
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
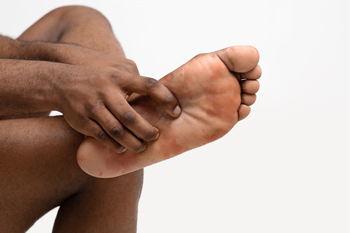
Pain on the bottom of the foot while walking can result from several conditions affecting the nerves, bones, and soft tissues. Metatarsalgia occurs when the ball of the foot experiences excessive pressure, leading to inflammation and discomfort. Peripheral neuropathy, often linked to diabetes, causes nerve damage that leads to tingling, burning, or sharp pain. Morton's neuroma is a thickening of nerve tissue between the toes, creating a sensation similar to stepping on a pebble. Additionally, sesamoiditis, an inflammation of the small sesamoid bones beneath the big toe, can cause pain with every step. If you have foot pain, it is suggested that you consult a podiatrist who can determine what the cause is, and offer effective relief and treatment solutions.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Richard DiMario from Maine. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Foot pain in children can result from overuse, wearing improper footwear, or underlying conditions affecting the feet, toes, or ankles. One of the most common causes of foot pain in children is Sever’s disease, medically known as calcaneal apophysitis, which occurs when repeated stress on the heel’s growth plate leads to inflammation. This condition often affects children ages eight to 14 involved in running or jumping sports like soccer or basketball. Another cause of childhood foot pain is Achilles tendonitis. This develops when the Achilles tendon becomes inflamed after increased activity levels, leading to heel pain, swelling, and difficulty walking. Foot fractures are another concern, particularly for children participating in high-impact sports. Fractures can cause intense pain, bruising, and an inability to bear weight. If left untreated, any of these conditions may worsen and interfere with your child’s daily activities. If your child complains of foot pain, especially after activity, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
The health of a child’s feet is vital to their overall well-being. If you have any questions regarding foot health, contact Dr. Richard DiMario of Maine. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tips for Keeping Children's Feet Healthy
If you have any questions, please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot care needs.
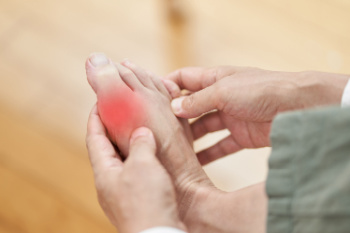
Gout, a form of arthritis caused by uric acid buildup in the joints, can be influenced by temperature and humidity. Cold temperatures may trigger gout attacks by causing uric acid to crystallize in the joints, leading to sudden pain and inflammation. High humidity can contribute to dehydration, which reduces the body’s ability to flush out uric acid, increasing the risk of flare-ups. Managing gout involves staying hydrated, maintaining a balanced diet, and avoiding triggers like alcohol and purine-rich foods. Wearing warm socks in cold weather and staying cool in hot, humid conditions can help prevent attacks. A podiatrist can help by recommending footwear and insulation strategies to protect joints from cold exposure. They may also provide guidance on proper hydration and lifestyle adjustments to minimize the impact of humidity. If gout affects your mobility or causes frequent flare-ups, it is suggested that you consult a podiatrist who can help you improve your comfort and overall foot health.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Dr. Richard DiMario from Maine. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Trail running shoes are designed for off-road running, offering essential features to enhance performance and comfort. One key feature is waterproofing, which helps keep feet dry in wet conditions, preventing discomfort and blisters during rainy runs or when crossing streams. For runners with wider feet, wide-fit trail running shoes provide extra space, ensuring a more comfortable fit and reducing pressure on the toes. Mud shoes are another important type of trail running shoe, equipped with specialized traction to handle slippery and muddy trails. These shoes typically have deeper treads that provide better grip and stability, preventing slips. Whether running through wet terrain, navigating rocky paths, or tackling muddy routes, the right trail running shoes ensure durability, support, and comfort for every adventure. If you have sustained a foot injury while trail running, it is suggested that you consult a podiatrist who can offer effective relief tips, and guide you on the correct shoes to wear.
If you are a runner, wearing the right running shoe is essential. For more information, contact Dr. Richard DiMario from Maine. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
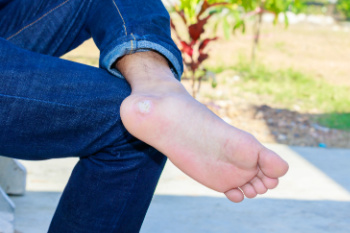
Plantar warts, or verrucas, are common viral skin growths caused by the human papillomavirus, or HPV. They often appear on the soles of the feet, especially in children, athletes, and those with weakened immune systems. The virus thrives in warm, moist environments like near pools, and in locker rooms and communal showers, spreading through direct contact. These warts may look like thick, rough calluses with tiny black dots, which are clotted blood vessels and can cause pain when walking. Over time, they may spread or cluster into mosaic warts. Stubborn plantar warts can persist. If you or your child has a plantar wart, it is suggested that you see a podiatrist who can provide prescription medications, laser therapy, or minor surgical removal.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Richard DiMario from Maine. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Foot and ankle swelling can occur for various reasons, often related to lifestyle, health conditions, or prolonged periods of immobility. One common cause is being overweight, as excess body weight places additional pressure on the feet and ankles, leading to fluid retention and swelling. Age is another factor, as older individuals may experience reduced circulation, which can contribute to swelling in the lower extremities. Leg infections can also cause swelling, as the body’s immune response leads to inflammation in the affected areas. Prolonged periods of immobility, such as on long airplane flights, can reduce circulation and lead to fluid buildup in the feet and ankles. A sedentary lifestyle, in which an individual remains seated or inactive for long stretches, can further cause swelling by preventing proper blood flow. If you have swollen feet or ankles, it is suggested that you confer with a podiatrist who can determine what the cause is, and offer appropriate treatment solutions.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Dr. Richard DiMario of Maine. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please feel free to contact our office located in York, ME . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.